Intraocular Lens (IOL) Exchange
When patients are not satisfied by the visual result after cataract surgery due to the lens that was placed in the eye, they may undergo referral for an intraocular lens exchange.
Call Us: 215-928-3180
When patients are not satisfied by the visual result after cataract surgery due to the lens that was placed in the eye, they may undergo referral for an intraocular lens exchange.
Call Us: 215-928-3180
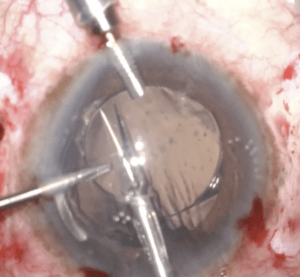 Intraocular lens exchanges may be considered in cases where visual acuity is not as expected, or if the patient experiences severe visual aberrations (such as glare, halos, or starburst) that have not improved with time or responded to more conservative measures. Some patients experience the latter symptoms after placement of a multifocal intraocular lens. Alternatively, if an intraocular lens is causing complications (such as by rubbing on the iris, causing eye inflammation), it may need to be removed and replaced with a new lens in a different location.
Intraocular lens exchanges may be considered in cases where visual acuity is not as expected, or if the patient experiences severe visual aberrations (such as glare, halos, or starburst) that have not improved with time or responded to more conservative measures. Some patients experience the latter symptoms after placement of a multifocal intraocular lens. Alternatively, if an intraocular lens is causing complications (such as by rubbing on the iris, causing eye inflammation), it may need to be removed and replaced with a new lens in a different location.
The risks associated with intraocular lens exchanges are generally higher than the initial cataract surgery, and there is a higher chance of corneal swelling, retinal swelling, and retinal breaks and detachments.
Depending on the anatomy of the eye and whether the “bag” that was holding the original lens is intact, the surgeon may decide to place the new intraocular lens directly into the “bag” that was holding the previous intraocular lens, or may position the new lens in other parts of the eye (e.g. in front of the “bag,” a region called the sulcus; or alternatively in front of the iris). When no “bag” is present, the surgeon may fixate a lens to the wall of the eye (called the sclera) or to the iris. Several techniques exist to fixate the lens to the eye, some involving and others without sutures.
The surgeon will usually pick a technique based on his/her experience. Sometimes, the jelly from the back of the eye (the vitreous) comes forward during the surgery, and the surgeon has to remove some of it (a procedure called a vitrectomy).
