Corneal Swelling after Cataract Surgery
Occasionally, after cataract surgery, the endothelial cells don’t function well enough to keep the cornea clear, causing poor vision and often discomfort
Call Us: 215-928-3180
Occasionally, after cataract surgery, the endothelial cells don’t function well enough to keep the cornea clear, causing poor vision and often discomfort
Call Us: 215-928-3180
The back layer of the cornea is made up of endothelial cells which keep the cornea clear. All cataract surgery (even “perfect” surgery) does some damage to these endothelial cells. Most corneas have plenty of “extra” endothelial cells, so a small degree of endothelial cell loss from cataract surgery doesn’t usually cause any problem. However, occasionally, after cataract surgery, the endothelial cells don’t function well enough to keep the cornea clear, causing poor vision and often discomfort. The cells may recover over the first few months after surgery.
If the cornea doesn’t clear, treatment options include:
• Drops to decrease swelling (saline-like drops) and corneal transplantation;
• Either a partial thickness corneal transplant (e.g. Descemet’s stripping endothelial keratoplasty [DSEK] or Descemet’s membrane endothelial keratoplasty [DMEK]), or a full thickness corneal transplant (especially in eyes with corneal scarring).
 DEFINITION
DEFINITIONCorneal swelling (edema) that develops after cataract surgery and doesn’t resolve over several months.
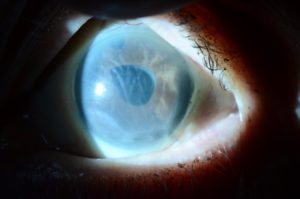
Blurred vision, may worse in the mornings, which may clear over a few hours, or may be present all day long. It often improves over the 1st few months after cataract surgery, but it may not. The swelling can cause painful blisters as the condition progresses.
Damage to the cells on the back layer of the cornea (endothelial cells) related to the cataract surgery. Even “perfect” cataract surgery can occasionally cause corneal swelling that doesn't resolve on its own.
History of Fuchs dystrophy prior to the cataract surgery is by far the most common risk factor for corneal swelling after cataract surgery. Other eye surgeries such as glaucoma surgery or retinal surgery, or prior eye trauma, also increase the risk of corneal swelling after cataract surgery.
Cornea scarring can develop in severe or longstanding cases.
The diagnosis can usually be made during a slit lamp examination. Ancillary testing can include measurement of the corneal thickness (pachymetry) and endothelial cell imaging (specular microscopy).
Treatment ranges from observation in mild cases to salt drops and ointment (hypertonic sodium chloride 5%) to surgery including partial thickness corneal transplant (e.g. Descemet’s stripping endothelial keratoplasty [DSEK] or Descemet’s membrane endothelial keratoplasty [DMEK]) or a full thickness corneal transplant (especially in eyes with corneal scarring).
Routine eye examinations are recommended to monitor the condition. Longstanding swelling increases the chances of developing corneal scarring which decreases the success rate of partial thickness corneal transplantation.
