Retinal Detachment
A retinal detachment is a separation of the retina from the underlying layers of the eye wall.
Call Us: 215-928-3300
A retinal detachment is a separation of the retina from the underlying layers of the eye wall.
Call Us: 215-928-3300
 The retina is the thin layer of tissue that retains the vision cells in the back of the eye—think of it as the film inside a camera. The image that one sees is focused by the lens and cornea in the front of the eye and then cast upon the center of the retina (macula) in the back of the eye.
The retina is the thin layer of tissue that retains the vision cells in the back of the eye—think of it as the film inside a camera. The image that one sees is focused by the lens and cornea in the front of the eye and then cast upon the center of the retina (macula) in the back of the eye.
Over time, retinal detachment will lead to progressive loss of peripheral and, eventually, central vision. Left untreated, total and permanent loss of sight eventually occurs in most cases.
A rhegmatogenous type of retinal detachment is caused by a break, tear or hole in the retina, allowing fluid from the vitreous cavity of the eye to track under the retina, detaching it from the eye wall. “Rhegma” is Greek for rent or break. Rhegmatogenous retinal detachment is the most common type of retinal detachment.
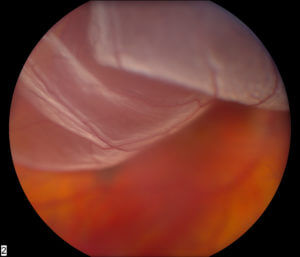
 Retinal tears and associated detachments of the retina are often spontaneous and unpredictable events. While detachment can arise following trauma, it is usually caused by separation of the vitreous gel from the retina. Over time as we age, the vitreous gel liquefies. It eventually collapses upon itself and separates from the surface of the retina (posterior vitreous detachment). During or shortly after this event, a retinal tear can occur as a result of the gel pulling on the thin retinal tissue.
Retinal tears and associated detachments of the retina are often spontaneous and unpredictable events. While detachment can arise following trauma, it is usually caused by separation of the vitreous gel from the retina. Over time as we age, the vitreous gel liquefies. It eventually collapses upon itself and separates from the surface of the retina (posterior vitreous detachment). During or shortly after this event, a retinal tear can occur as a result of the gel pulling on the thin retinal tissue.
Risk factors for developing retinal tears and detachment include myopia (near-sightedness), particularly thin patches within the peripheral retina (lattice degeneration), family history, previous eye surgery, and trauma.
The rate of progression of a retinal detachment can vary from days to weeks depending on many factors such as patient age as well as the size and the number of retinal tears.
Symptoms of vitreous detachment, retinal tear, and retinal detachment may coexist and include:
A comprehensive ophthalmic examination is essential to diagnose and treat a retinal detachment. Through a dilated pupil, the ophthalmologist will see one or more tears in the retina with varying amounts of underlying fluid. There may also be some degree of vitreous hemorrhage, which occurs when a retinal tear involves a retinal blood vessel.
Retinal detachments often cause some degree of permanent visual field or central visual acuity loss, even after successful reattachment. Final visual outcomes are best if the detachment is detected and treated before it involves the center of the retina (macula). A change of eyeglasses after retinal detachment surgery may or may not improve vision. Longstanding retinal detachments or those with associated scar tissue (proliferative vitreoretinopathy) typically have a poor visual prognosis.
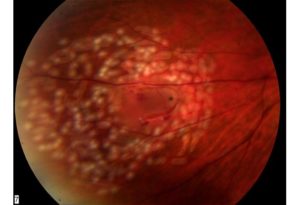
If a retinal hole or tear is detected before there is retinal detachment, laser or cryotherapy (freezing treatment) to the retinal tear is often successful in sealing the retinal defect, preventing a retinal detachment. However, if a retinal detachment has already developed, a retinal reattachment procedure is typically necessary.
There are three approaches to repairing a retinal detachment:
The choice of treatment depends on certain features of the detachment such as number and location of retinal tears as well as patient characteristics such as age and past cataract surgery.
Pneumatic Retinopexy is an office-based procedure. It involves the injection of a temporary gas bubble to close the retinal tear and surrounding detachment. The gas injection is coupled with either a freezing treatment (cryotherapy) or laser photocoagulation to permanently seal the causative retinal tear. After the procedure, patients must maintain a specific head position for about a week to ensure that the retinal tear is adequately sealed
Scleral buckle surgery is performed in the operating room. It consists of suturing a soft piece of silicone to the eye wall (sclera) in such a way as to gently indent the sclera in order to support and close the retinal tear. It is coupled with either cryotherapy or laser photocoagulation. A gas bubble is sometimes used to facilitate reattachment of the retina. In some cases, a scleral buckle may be combined with vitrectomy surgery.
Vitrectomy surgery is also performed in the operating room. As the name implies, it involves surgical removal of the vitreous gel which, in turn, relieves the traction or pulling on the retinal tear that is causing the detachment. Laser is then used to seal the retinal tears. Lastly, the eye is filled with either gas or silicone oil. Gas goes away slowly on its own, but oil does not. Silicone oil may be removed at a later date with another vitrectomy. (The use of silicone oil is usually reserved for complex retinal detachments such as those with associated scar tissue or very large retinal tears.)
