Corneal Transplantation
A corneal transplant, also known as keratoplasty, is a surgery that replaces a damaged or diseased cornea with a healthy donor cornea to restore vision.
Call Us: 215-928-3180
A corneal transplant, also known as keratoplasty, is a surgery that replaces a damaged or diseased cornea with a healthy donor cornea to restore vision.
Call Us: 215-928-3180
Your cornea must be clear, smooth and healthy for good vision. If it is scarred, swollen, or damaged, light is not focused properly into the eye. As a result, your vision is blurry or you see glare.
If your cornea cannot be healed or repaired, your ophthalmologist may recommend a corneal transplant. This is when the diseased cornea is replaced with a clear, healthy cornea from a human donor.
There are different types of corneal transplants as listed below. In some cases, only the front and middle layers of the cornea are replaced. In others, only the inner layer is removed. Sometimes, the entire cornea needs to be replaced.

VIDEO: Wills Eye cornea surgeon Zeba. A. Syed, MD explains corneal transplantation.
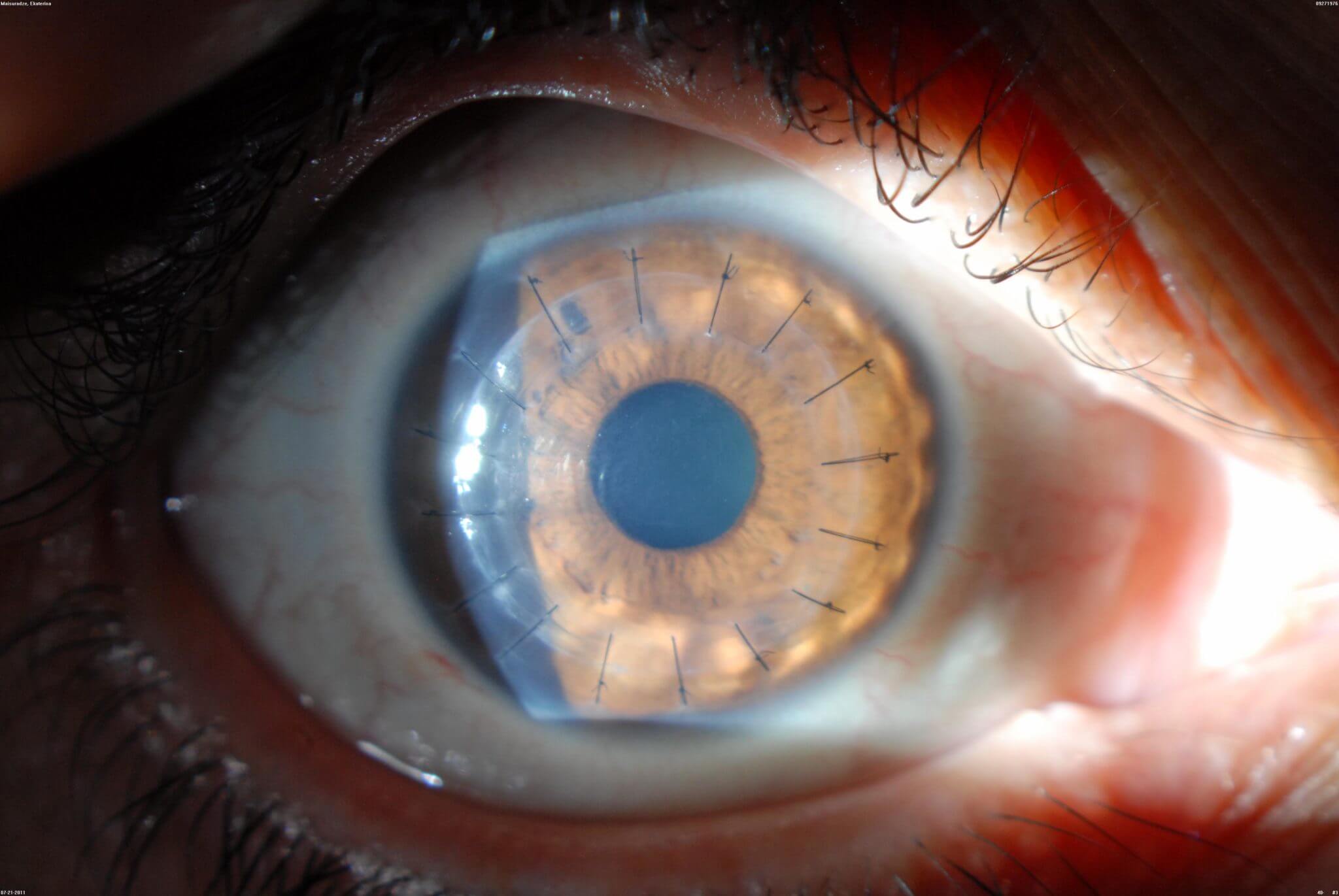
This type of corneal transplant is performed when both the front and back layers of the cornea are abnormal. It involves using a blade to remove most of the cornea and a new human donor cornea is sutured into place.
Advantages of this type of transplant include replacement of all layers of the cornea, a long successful track record, fairly straightforward surgery, and ready access to perform surgery inside of the eye. Disadvantages include a relatively long visual recovery period, a large wound with many sutures, possible high degree of astigmatism, and unpredictable post-operative refraction. Corneal transplantation is performed using local or general anesthesia in the operating room.
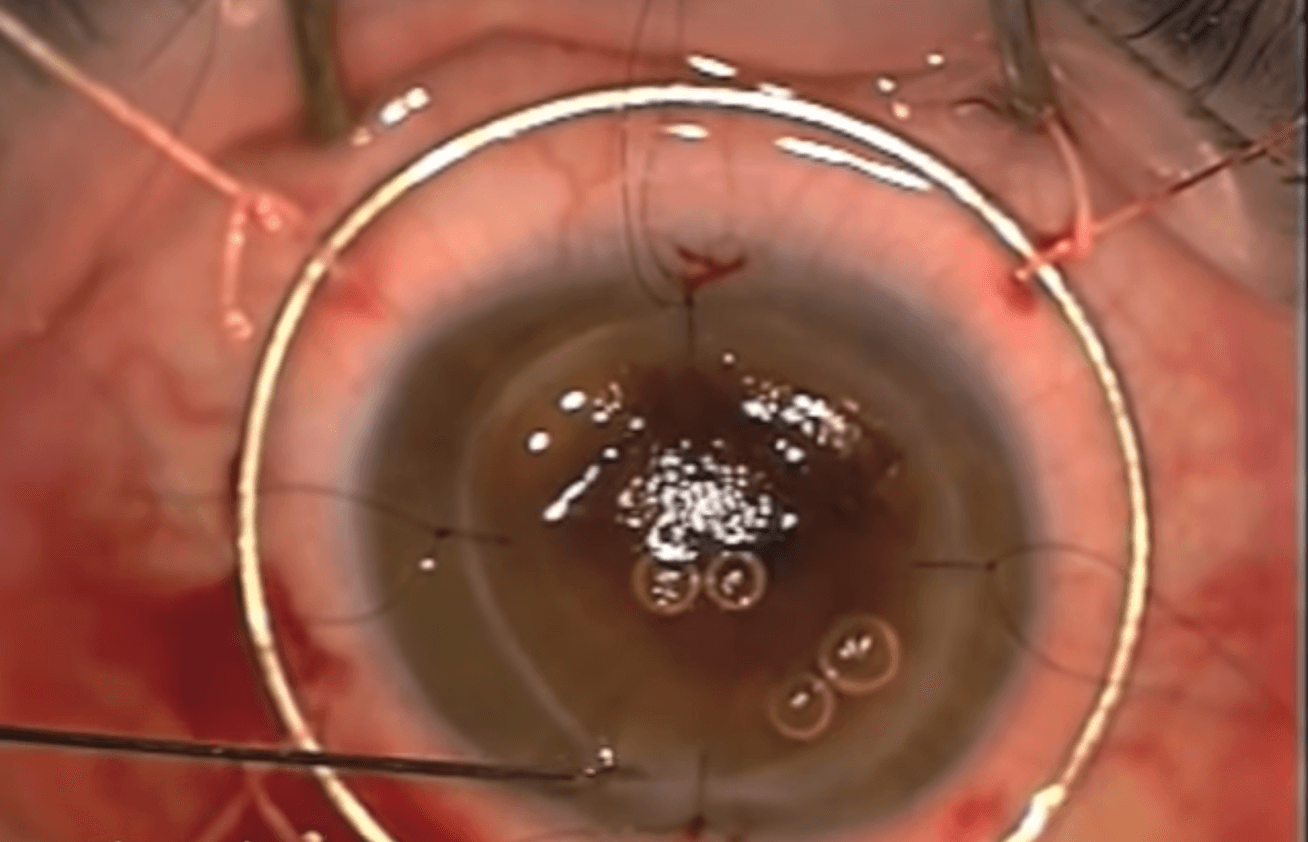
The back layers of the cornea are the endothelium and Descemet’s membrane. Endothelial cells pump fluid out of the cornea to keep it clear to maintain good vision. When these cells aren’t functioning, the cornea becomes swollen. This may be seen in conditions such as Fuchs dystrophy and after cataract surgery. If there isn’t significant scarring in the front of the cornea, DSEK or DMEK can be performed to replace these cells to clear the cornea.
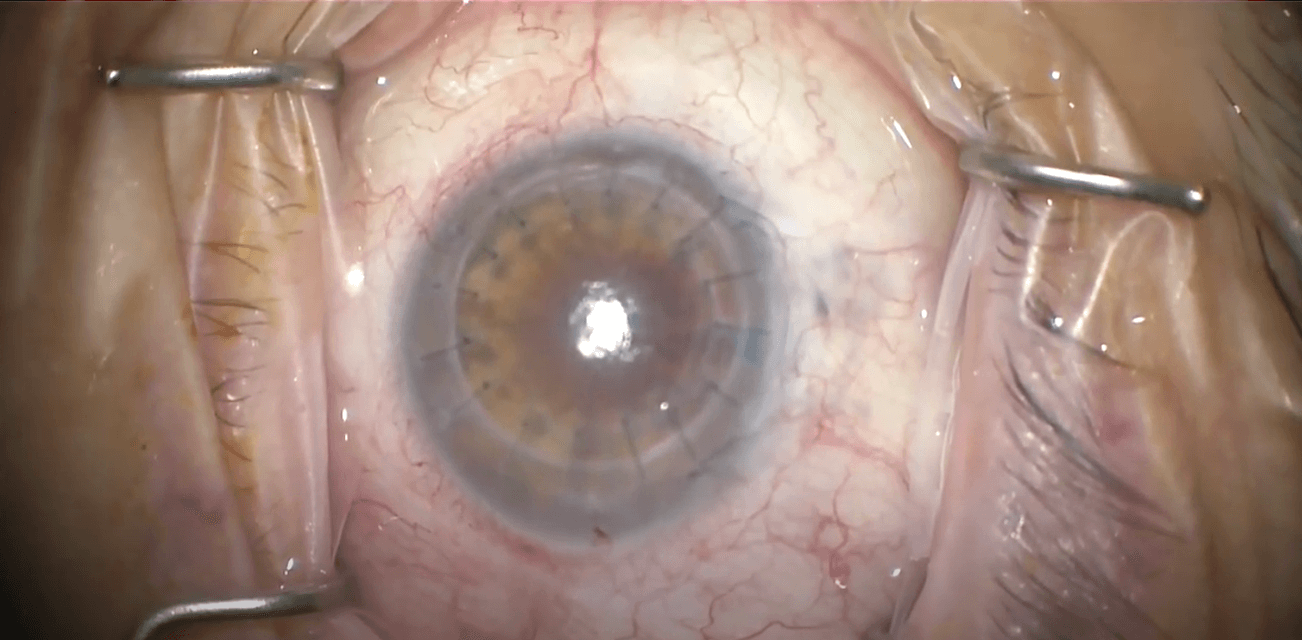
This surgery involves removing the damaged endothelial cells and Descemet’s membrane and replacing it with partial thickness graft including donor endothelium and Descemet’s membrane. The surgery is performed through a small incision, requiring that the graft be folded or rolled to get it into the eye. It is then held into position with an air bubble or special gas for a period of time, after which (most of the time) it adheres.
Advantages include a small incision with few or no sutures, faster visual recovery than after PK, and minimal change in astigmatism or post-operative refraction. Disadvantages include the fact it is newer surgery and that the graft occasionally does not adhere, requiring further surgery.
When Fuchs dystrophy is central and mild, DSO may be performed. In this procedure, only the diseased cells are removed and no tissue is placed into the eye. Your “healthy” cells are given a chance to fill in the space that remains after removing diseased cells. Sometimes your surgeon may use a special drop to help your own cells “fill in” the gaps. DSEK, DMEK, and DSO are performed using topical, local, or general anesthesia in the operating room.
When the problem in the cornea involves the body of the cornea (stroma), and the back layers of the cornea (Descemet’s membrane and endothelium) are healthy, a DALK can be attempted.
This procedure is similar to a full thickness corneal transplant with the exception that the patient''s own back layers (Descemet’s membrane and endothelium) are not removed or replaced. The main advantage is less risk of transplant rejection. When DALK is attempted, there is a reasonable chance that the very thin back layers of the cornea tear during the surgery, at which point a full thickness corneal transplant is typically performed.