Trabeculectomy Surgery
Trabeculectomy is a glaucoma surgery designed to improve fluid drainage from the eye, thereby lowering eye pressure and reducing the risk of damage to the optic nerve.
Call Us: 215-928-3197
Trabeculectomy is a glaucoma surgery designed to improve fluid drainage from the eye, thereby lowering eye pressure and reducing the risk of damage to the optic nerve.
Call Us: 215-928-3197
Trabeculectomy: A Glaucoma Surgery to Lower Eye Pressure
A trabeculectomy is a glaucoma operation that has been used successfully for many years. In the United States, it is common to treat glaucoma with medicines and laser first, and then move on to surgery. When these measures fail or cannot be used, trabeculectomy is often the recommended next step. This surgery is designed to significantly lower the fluid within the eye to lessen the likelihood of pressure damage to the optic nerve, which transmits vision from the eye to the brain. Although no surgery can cure glaucoma permanently or reverse vision loss that has already occurred, trabeculectomy is often effective in controlling pressure and reducing the risk of additional vision loss for several years in the majority of patients.
How does the trabeculectomy work?
A trabeculectomy creates a new passageway for the fluid that the eye produces to leave the eye more easily and be reabsorbed by the tissues surrounding the eye. Sometimes healing and scar tissue can reduce flow through the new drainage channel. Medications applied at the time of the operation, or used in the office shortly after the surgery help to prevent the scar tissue from forming. There are also special devices that can be used along with a trabeculectomy surgery to try to maintain the passageway for and regulate the rate of fluid escape.
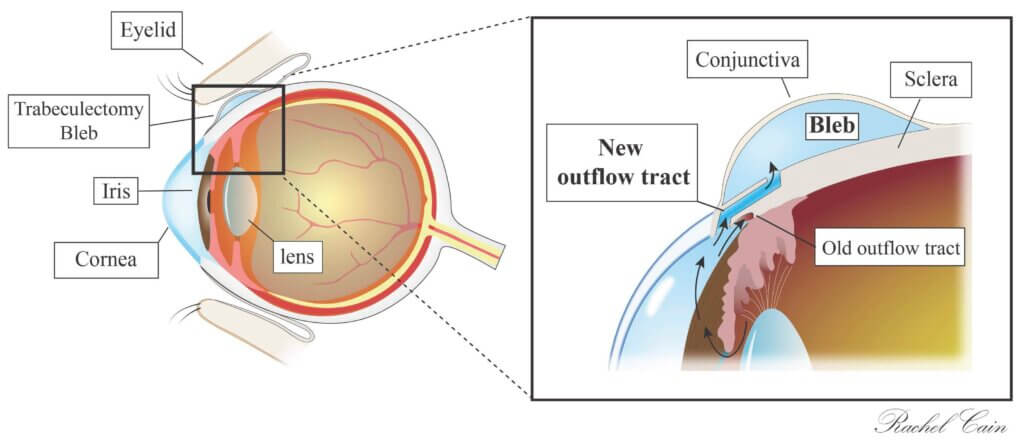
What are the steps of surgery?
The surgery is performed in the operating room. Your eye will be numbed with eye drops and numbing jelly. The anesthesiologist will give you medications through your IV to keep you relaxed and calm during surgery. The eye is cleaned and the face will be covered with a sterile drape. An instrument opens the eyelids.
What happens to the eye after surgery?
Once the trabeculectomy has been created, fluid begins to use the new passageway to leave the eye more easily. This escaping fluid raises the filmy skin covering the surface of the eye creating a "filtering bleb." This "bleb" or bubble on the surface of the eye is usually under the upper eyelid so it is not visible without raising the upper lid. The fluid is reabsorbed from the bleb by the tissues and veins around it. Many patients require a short laser procedure in the office after surgery to break the sutures to the edge of the flap. This laser allows the trabeculectomy to work better.
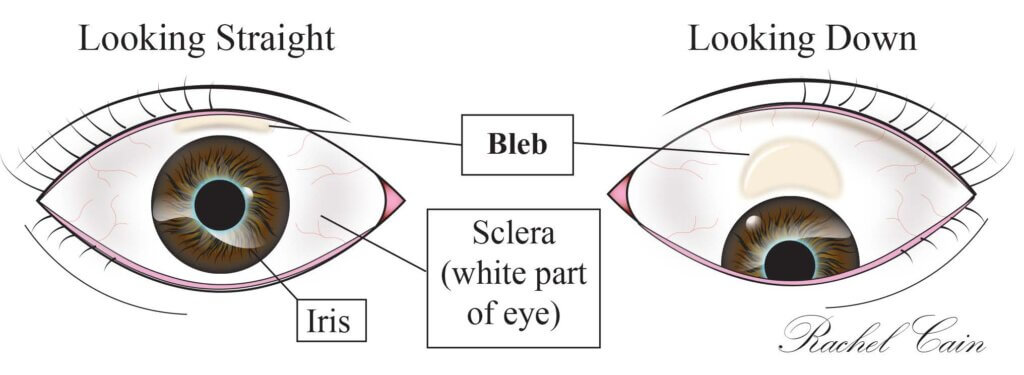
With a successful trabeculectomy, the eye pressure can be lowered for several years. The patient's age, type of glaucoma, and many other factors play a part in the success of the procedure. Some patients may have extra scar formation which can block the passageway. Because there is no effective way to monitor healing and eye pressure at home, it is very important to keep follow-up appointments. This gives your surgical team the chance to see you often, monitor the pressure and the healing, watch for complications, and give you the best chance for a positive result. The need for glaucoma eye drops is usually reduced or eliminated after surgery.
What will I feel during and after the surgery?
You may see bright lights during the surgery, but should not feel any pain. You will be discharged with a clear plastic shield with or without a patch over the operated eye. An adult will need to drive you home since you received sedating medications.
How often will I be seen after surgery?
You will see your doctor the first day after surgery, about a week later, and a few weeks after that. Depending on how your eye heals, additional or fewer visits may be needed.
What eye drops will I use after surgery?
Most patients will be asked to use a steroid and antibiotic eye drops. The frequency of the taking the steroid eye drops depend on the amount of the eye inflammation.
Can I stop my glaucoma drops after surgery?
Your doctor will tell you which drops to continue using and how often at each visit depending on how your eye is doing. Sometimes patients are able to reduce the number of eye drops they are taking. Even if you are taking the same glaucoma medications after the procedure, the surgery is a success if your pressure is lower.
Will my vision improve right after surgery?
The first few days after surgery, vision may be blurry and even worse than it was before surgery. This will improve over several weeks, although it can sometimes take longer. The eye that was not operated on will not be affected, and may be depended on for vision during the recovery period (if it has vision).
What is the recovery time and what should I expect?
Depending on your job and your other eye, you should be able to return to work within a few days to a few weeks. Limitations in physical activities at work may be needed. After surgery, your eye may be sore, and it may feel like there is something in it, like an eyelash. The drops may burn when you put them in, and your eye may water or tear a lot. These symptoms are common but usually are mild, and improve for most people after 1-2 days. Tylenol (acetaminophen) is a good option unless you are unable to take this medication. If your eye has severe pain or sudden worsening pain or vision after surgery, please call our office or on call physician immediately.
Will I have any restrictions after surgery?
You will be given detailed instructions after your surgery that are specific to your eye’s needs. In general, the following guidelines apply:
There are no restrictions in reading, watching TV, using your phone, tablet device, computer, etc but you may tire more easily during these activities.
Will Trabeculectomy cure my glaucoma?
The simple answer is “no”. Glaucoma is a chronic disease that requires constant monitoring and treatment. The trabeculectomy procedure will help to lower your eye pressure. However, it will not reverse any loss of vision that has already occurred.
What are the possible side effects of trabeculectomy surgery?
Possible complications may include, infection, bleeding in the front or back part of the eye, buildup of fluid between the choroid (inner layer of blood vessels) and the sclera (white outer layer of the eyeball), very low eye pressure, wound leak, need for additional surgical intervention, and other eye surgery complications. In some patients, the eye pressure may increase and an additional surgical procedure in the eye to release scar tissue (needling) at the site of the surgery may be required. However, for many patients, the risk of surgery is lower than the risk of losing vision from glaucoma.
What happens if trabeculectomy does not work?
In case of early failure, breaking the scar at the site of surgery and injection of the anti-scar medication may restore the flow. Starting or adding glaucoma medications may keep your eye pressure controlled. If trabeculectomy fails and eye pressure is elevated despite using glaucoma medications, the surgical revision of the surgery site to remove the formed scar tissue, tube shunt surgery, and a specific type of laser (cyclophotocoagulation) can be employed to lower the eye pressure.
For more information, please see:
Wills Eye Hospital Glaucoma Website:
www.willseye.org/glaucoma
American Academy of Ophthalmology Patient Information Website:
https://www.aao.org/eye-health/diseases/what-is-glaucoma
American Glaucoma Society Patient Information Website:
https://www.americanglaucomasociety.net/patients/patient-education
